Quality-focused news brief with shocking findings presented at two major conferences, and more recent stories you might have missed on MitraClip results and PCI strategy. Does MitraClip produce positive results, or not? Should CTCA be the first-line imaging test for stable chest pain? And what “tools and tricks” improve outcomes in PCI?
MitraClip Reduces Hospital Stays, Deaths Among Patients With Heart Failure – AJMC In Focus Blog
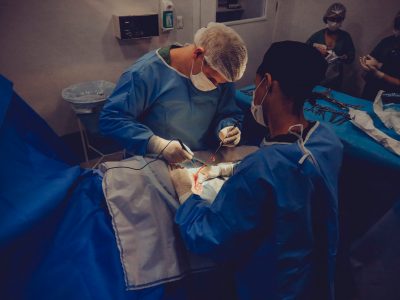
MitraClip results from the COAPT trial, funded by Abbott, shocked physicians at TCT2018, showing that transcatheter mitral valve repair with MitraClip dramatically improved “survival, quality of life, and the ability of patients with heart failure to function.” An earlier study in Europe did not produce positive results. Read more »
SCOT-HEART: CT Angiography Linked to Less Death, Nonfatal MI in Stable Chest Pain – Medscape
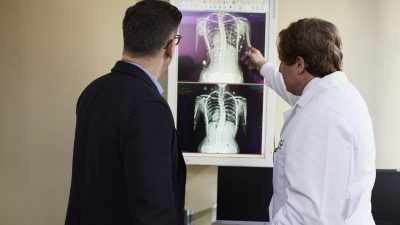
Surprising findings from TCT2018 reminded us of this story from late August out of the ESC Congress 2018—one that also surprised many physicians. The SCOT-HEART trial showed that CT coronary angiography (CTCA) for patients with stable chest pain “leads to a significant reduction in rates of death from coronary heart disease (CHD) or nonfatal myocardial infarction (MI) after 5 years, without increasing coronary intervention rates.” No other imaging test is shown the reduce the rates of MI, explains David E. Newby, MD, who led the study. “So why aren’t we using it first line?” he asks. Read more »
‘Enabling Strategies’ Improve Success of Chronic Total Occlusion PCI – TCTMD
Volume and experience aren’t the only factors that improve procedural success rates in chronic total occlusion PCI—several tools and tricks also contribute significantly to quality according to registry data presented at TCT 2018. These ‘enabling strategies’ include: “IVUS, rotational/laser atherectomy, dual arterial access, and use of microcatheters, penetration catheters, or CrossBoss (Boston Scientific).” Read more »
TCT.18: Pre-PCI statin dose slashes MACE by 28% – Cardiovascular Business
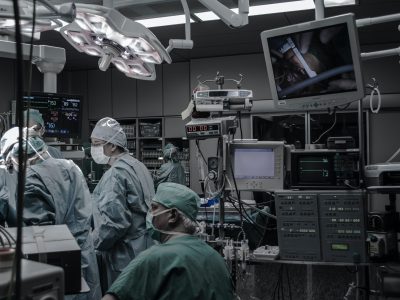
Secondary analysis of the randomized SECURE-PCI trial suggested that a pre-PCI statin dose for acute coronary syndrom patients resulted in “a 28 percent reduction in major adverse cardiovascular events (MACE) over the following 30 days.” One of the key messages, says lead author Renato D. Lopes, MD, is that “we’re going to have to give statins no matter what in some high-risk patients, [so] why not just give it up front and potentially save the events with the 30-day follow up.” Read more »